This article contains affiliate links. If you make a purchase after clicking on a link I may earn a small commission at no extra cost to you.
Who Is At Risk?
Roughly 1 percent of the North American population is at risk of anaphylaxis.
Near-fatal or fatal anaphylactic episodes are most common among adults, although children may be at as great, or greater, risk because of their inability to recognize and act on the emergency. In children, anaphylactic episodes tend to produce fewer cardiovascular (blood system and heart) problems and more airway obstruction, swelling and hives.
People who are taking beta-blocker drugs for high blood pressure or other disorders are at increased risk of anaphylaxis, because they will not respond to epinephrine injected as an antidote.
If you have experienced allergic reactions, you may be advised to use other drugs instead of beta blockers.
Living with the Risk of Anaphylaxis
The management of anaphylaxis depends primarily on the three “A’s”: Awareness, Avoidance and Action (i.e., epinephrine injection).
Once the allergen has been pinpointed, avoidance is the key — especially being alert to hidden or accidental exposures.
People must be fully informed about the severity of their allergy and have it evaluated by a reliable allergist, and must learn the correct emergency measures. While the best course for preventing anaphylaxis is obviously to avoid triggers — such as lobster, wasps or penicillin — the next best is to prepare ahead for a possible attack with a pocket self-injection kit — such as Ana-Kit, EpiPen or Ana-Guard — available by prescription.
One injection may be enough, but a second dose, and even subsequent doses, may be needed 10 to 20 minutes later.
People known to be at risk should also wear a medical-alert bracelet or necklet clearly stating “risk of anaphylaxis,” the substance(s) to which they are allergic and the fact that they carry an injection kit. In addition, they should be sure the people around them — friends, relatives, co-workers — know what to do if they find someone in anaphylactic shock.
Taking preventive antihistamines (especially long-acting forms) before entering a situation with an exposure risk —going to a party, eating at a restaurant — may occasionally lessen the severity of an attack.
But this practice is controver-sial; many experts believe that premedication masks the early warning signs of anaphylaxis (such as the hives and swelling or flushing), and may let the condition become very severe before the danger is recognized.
“It cannot be emphasized enough,” states one expert, “that epinephrine is the only proper treatment for anaphylaxis. Antihistamines take from half an hour to two hours to work and cannot save a life. Antihistamines are not a substitute for epinephrine; they are not strong enough to treat anaphylaxis, although they can be helpful in controlling the symptoms.”
EpiPen Emergency Kits Save Lives
Some self-injector kits, such as the EpiPen, automatically inject a life-saving dose of epinephrine when the tip is pushed hard on the skin of the outside upper thigh. 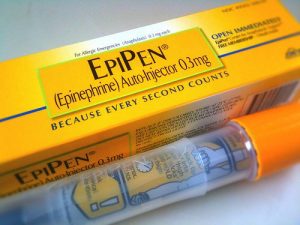
These are very easy to use. (An EpiPen Junior is available for children under 33 pounds — 15 kilos — in weight.)
Other kits, such as the Ana-Kit, contain a preloaded syringe and needle that must be injected in the usual manner. A special plunger ensures that only one dose is injected at a time.
Kits should be kept out of direct sunlight, which may affect the drug, and very hot or cold conditions.
Expired kits should be replaced.
All too often, people who have been prescribed self-injector kits don’t have a kit on them when it’s needed. They may be caught off guard, perhaps stung by a wasp at the pool, or unknowingly eating a bit of shrimp or peanut at a party, putting their lives in jeopardy.
That’s why, if you need a kit, you should always have it with you. Remember, though, that emergency injection is no substitute for medical help. It just “buys you time” until you can reach a physician or hospital.
